 
2010 report from the Center for International Blood and Marrow Transplant Research (CIBMTR): current uses and outcomes of hematopoietic cell transplants for blood and bone marrow disorders. Pasquini MC, Wang Z, Horowitz MM, Gale RP. Immunological reconstitution of sex-linked lymphopenic immunological deficiency. Gatti RA, Meuwissen HJ, Allen HD, Hong R, Good RA. Intravenous infusion of bone marrow in patients receiving radiation and chemotherapy. THOMAS ED, LOCHTE HL, LU WC, FERREBEE JW. Treatment of murine leukaemia with X rays and homologous bone marrow preliminary communication. This is a regimen that comprises high-dose chemotherapy and/or total body irradiation (TBI) which are administered to the recipient prior to stem cell infusion to eliminate the largest number of malignant cells and to allow for immunosuppression in the recipient so that engraftment can occur.Ĭopyright © 2023, StatPearls Publishing LLC.īARNES DW, CORP MJ, LOUTIT JF, NEAL FE. The process of which infused transplanted hematopoietic stem cells produce mature progeny in the peripheral circulation The donor is an HLA matched family member, unrelated matched donor or mismatched family donors (haploidentical). The disadvantage is that the bone marrow products may contain abnormal cells that can cause relapse in the case of malignancy hence theoretically, this method cannot be used in all cases of abnormal bone marrow diseases. 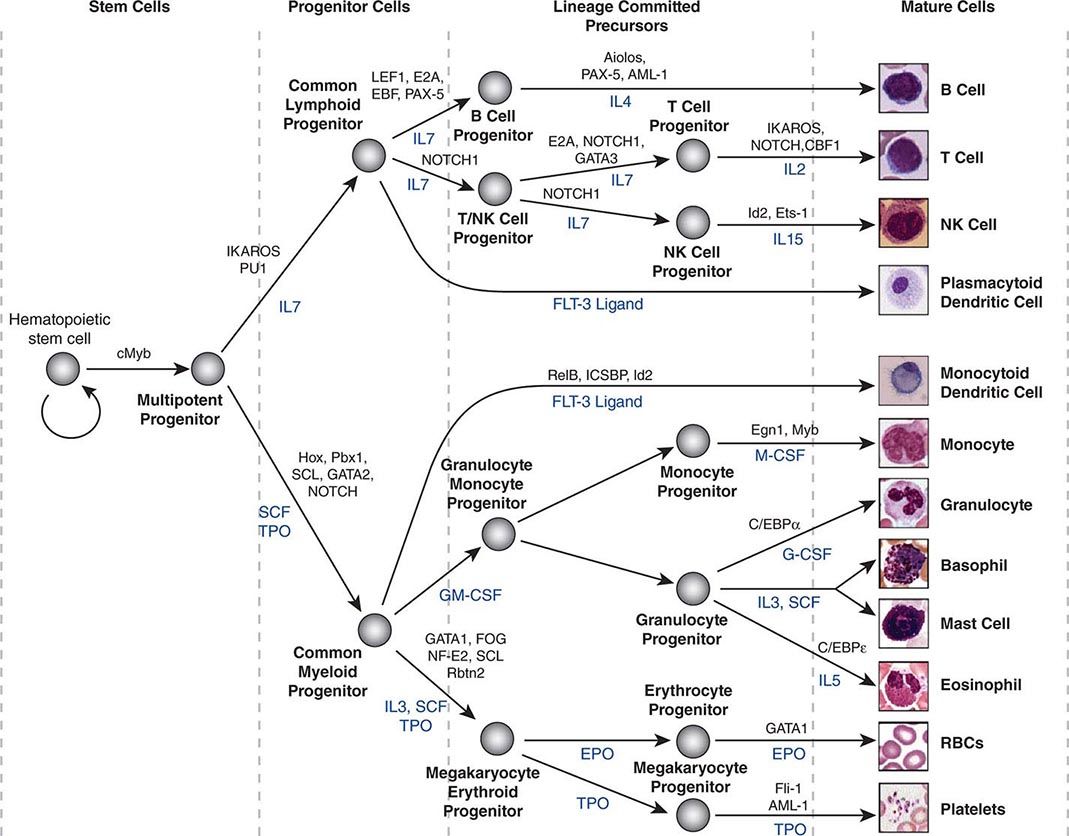
The bone marrow products are collected from the patient and are reinfused after purification methods. However, only a tiny number of transplant patients will have the ability to have an identical twin for transplantation. The advantages include no graft versus host disease (GVHD) and no graft failure. The donor and the recipient are identical twins. The other HLA type is classified as (HLA- DP, DQ, and DR) which are encoded by MHC II and can be found on antigen-presenting cells (APCs) and this class is recognized by CD4+ T cells. HLA can be divided into (HLA-A, B, and C) which are encoded by class I MHC and are expressed on all cell types and present peptides derived from the cytoplasm and are recognized by CD8+ T cells. These are the proteins expressed on the cellular surface and play an important role in alloimmunity. The group of genes on the short arm of chromosome 6 (p6) that encodes human leukocyte antigens (HLA) which are considered being highly polymorphic leading to a large difference in the resultant expressed proteins on human cells. The Center for International Blood and Marrow Transplant Research (CIBMTR) reported over 8000 allogenic transplants performed in the United States in 2016 with a higher number of autologous transplants with a steady and higher increase of autologous compared to allogenic. Since then, allogeneic and autologous stem cell transplant has increased in the United States and worldwide. The first successful allogeneic bone marrow transplant was reported in Minnesota in 1968 for a pediatric patient with severe, combined immunodeficiency syndrome. Thomas who performed the procedure continued his research on the development of bone marrow transplantation and later received the Nobel Prize of physiology and medicine in appreciation of his work. These animal-based studies soon found their clinical application into humans when the first successful bone marrow transplant was performed in monozygotic twins in New York in 1957 (syngeneic transplant) in a patient with acute leukemia. Hematopoietic stem cell transplantation (HSCT) was first explored in humans in the 1950s and was based on observational studies in mice models which showed that infusion of healthy bone marrow components into a myelosuppressed bone marrow could induce recovery of its function in the recipient. This helps to augment bone marrow function and allows, depending on the disease being treated, to either destroy tumor cells with malignancy or to generate functional cells that can replace the dysfunctional ones in cases like immune deficiency syndromes, hemoglobinopathies, and other diseases. Bone marrow transplant (hematopoietic stem cell transplant) (HPSCT) involves the administration of healthy hematopoietic stem cells in patients with dysfunctional or depleted bone marrow. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
